 |
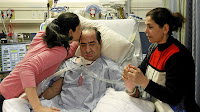
| Rasouli Family |
The Rasouli case is based on a dispute between the doctors and the family. The doctors at Sunnybrook hospital claimed that Hassan Rasouli was in a Persistent Vegetative State (PVS) and they state that they have the right to withdraw the ventilator from Mr. Rasouli without consent.
The Rasouli family objected to withdrawing the ventilator based on two grounds:
1. the Rasouli family are Muslim and they have religious objections to withdrawing the ventilator;
2. his wife, a physician, did not agree that her husband was in a PVS state.
The Euthanasia Prevention Coalition (EPC) intervened in the Rasouli case at the Ontario Court of Appeal, because we believe it is not safe to give doctors the unilateral right to withdraw life-sustaining medical treatment. The three judge panel, from the Ontario Court of Appeal, unanimously agreed that doctors were required to obtain consent before withdrawing life-sustaining treatment. The doctors appealed the unanimous decision of the Ontario Court of Appeal to the Supreme Court of Canada. EPC has requested to intervene in the Rasouli case at the Supreme Court of Canada.
The article by Lisa Priest that was published in the Globe and Mail indicates that Hassan Rasouli is now giving 'thumbs up' and responding to people's commands. His doctors have determined that he is not in a PVS state and the family has asked the Supreme Court of Canada to quash the case.
The article says:
A hospital patient deemed vegetative is now able to make a “thumbs up” gesture – a sign to family that he is aware, but not yet strong enough to persuade doctors to drop a recommendation to withdraw life support.Link to previous articles about the Rasouli case. Link.
The symbol marks a dramatic turn for Hassan Rasouli, 60, who until recently was in a persistent vegetative state. An affidavit filed with Canada’s top court says he’s now minimally conscious, and doctors’ reports say he can “voluntarily control” certain behaviours – suggesting he may be aware but trapped in a paralyzed body.
This new diagnosis seems certain to inflame an already divisive ethical debate about who decides to withdraw life support. And it raises the discomfiting notion – the stuff of relatives’ nightmares – of a patient being aware but unable to communicate when the machines are turned off.
“He is still there,” Mojgan Rasouli, 29, said of her father who has been at Toronto’s Sunnybrook hospital since October, 2010, after sustaining a brain infection after surgery for a brain tumour. “He can feel us and we can feel him.”
The case before the Supreme Court of Canada was begun by two doctors from Sunnybrook Health Sciences Centre, Brian Cuthbertson and Gordon Rubenfeld, who saw no medical purpose in keeping Mr. Rasouli on life support and proposed shifting him to palliative care.
The affidavit, filed by Dr. Cuthbertson, chief of critical care at Sunnybrook, spawned activity in and out of the courtroom. Gary Hodder, lawyer for the Rasouli family, filed a motion to quash the appeal as moot. A leading neuroscientist, Adrian Owen, travelled to Mr. Rasouli’s bedside at Sunnybrook on Tuesday, to conduct investigations to determine whether he can communicate.
His investigations come on the heels of a study he published in the medical journal The Lancet, revealing that 19 per cent of patients believed to be in an irreversible vegetative state showed signs of full consciousness when tested with an electroencephalography machine.
This is a murky area. Medicine is as much art as science, and sometimes even the most seemingly hopeless of patients experiences a change in condition. Whether Mr. Rasouli can communicate is a crucial question on which the medical case is expected to turn.
If he can, he “may be able to, or even capable of, expressing end-of-life wishes, such as whether to discontinue life support,” said Mark Handelman, an expert in health-care law.
If he cannot, Dr. Cuthbertson and other treating physicians “remain of the view that the standard of care does not require continuation of mechanical ventilation given his condition,” the affidavit says. It says Mr. Rasouli has also been diagnosed with other conditions, including spastic quadriplegia, which are extremely unlikely to improve in the long term.
Mr. Rasouli, a retired engineer, receives round-the-clock care: A mechanical ventilator does his breathing; a tube inserted into his stomach provides nutrition and fluids, while a catheter drains his urine. Medications maintain his blood pressure and he must be turned to prevent bed sores.
Sunnybrook neurologist Richard Swartz initially diagnosed him to be in a persistent vegetative state. But he noted things had “clearly changed” when he assessed Mr. Rasouli in late January, nearly 11 months from his last visit.
The patient was “consistently able to show a ‘thumbs up’ ” to verbal requests, with his wife, Parichehr Salasel, translating to Farsi. “… Importantly, he has consistently shown visual pursuit, one of the earliest signs of MCS [minimally conscious state].”
Lawyer Harry Underwood, who represents critical-care physicians Dr. Cuthbertson and Dr. Rubenfeld, declined comment. Dr. Swartz could not be reached.
Mr. Hodder said the new diagnosis “changes the entire texture of the situation. We’re now talking about someone who has some degree of consciousness.”
Bernard Dickens, professor emeritus of health law and policy at University of Toronto, says if it turns out Mr. Rasouli is aware, his lawyers could argue that disconnecting him from life support would cause him moral anguish and could violate the “do no harm” oath of physicians.
For the Rasouli, family, however, this is important not only personally but for other patients facing the same painful issue.
“This could help other families, future patients,” Ms. Rasouli said. “Maybe some families give up. Everything is possible.”
Link to a previous article explaining the Rasouli case. Link.

2 comments:
Here some important information:
http://www.spkpfh.de/The_medical_doctors_prey_on_body_organs.htm
http://www.spkpfh.de/Diapthics%20of%20a%20Resurrection.htm
Thanks for great information you write it very clean. I am very lucky to get this tips from you.
Foot Protectors Bed Sores
Post a Comment